|
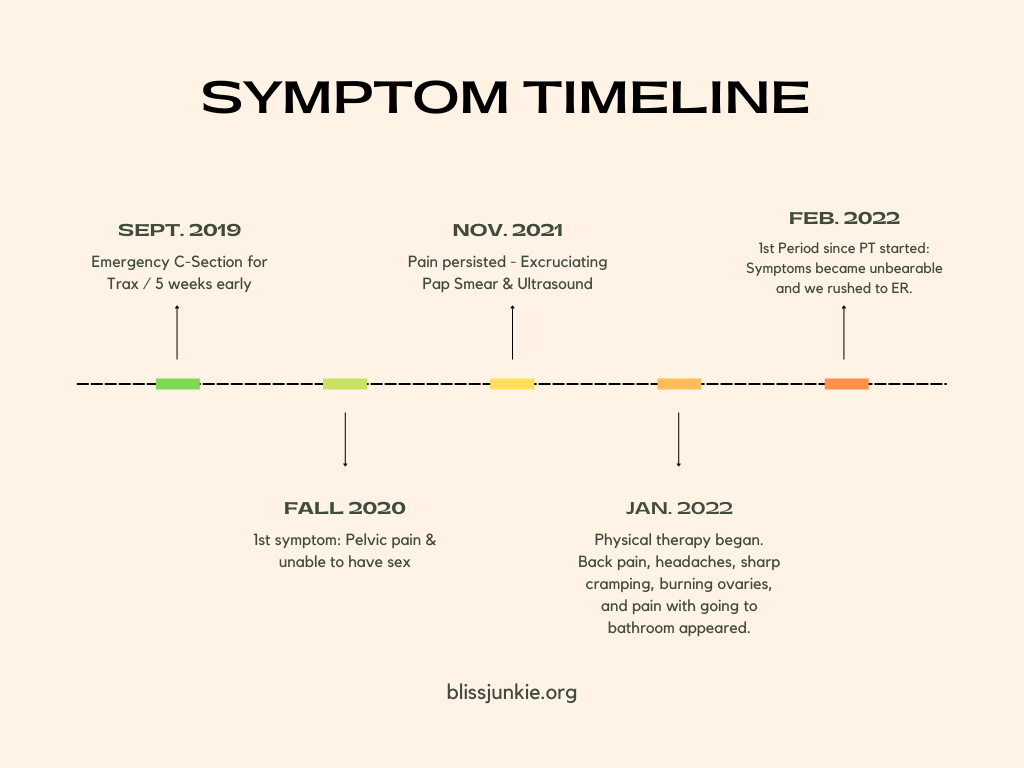
My knees were tucked up to my chin and the tie dye comforter was clenched in my knuckles. I squeezed my eyes and thanked God we had a babysitter to watch Trax. As I buried my face into a pillow, the sharp cramping in my pelvis turned into a pulsing stab. I texted my husband at work and said we may need to go to the ER. I deleted the words as soon as I finished them. Maybe I can swig another ibuprofen and wait this out. After I took the pill, I headed to the closet to change clothes just in case. Another bolting cramp made me sink down the wall to the floor. Once it passed, I wobbled back over to my phone and rewrote the text. Send. Hey y’all. It’s been a minute. I took a handful of months off writing while I was in and out of the hospital. I’m happy to be back though :) I missed writing. Let’s jump back into my first ER visit… That was my first trip to the ER, which was roughly five weeks after my OBGYN told me I might have Endometriosis. The fall of 2020, I started experiencing rough pelvic pain, which also meant I could not have sex. As November of 2021 arrived, the pain persisted and that area of my body became sore to the touch. I had also received an abnormal pap smear in 2019 when I was pregnant with my son and they suggested retesting in the future. So, I scheduled a yearly pelvic exam, unaware of how long my doctor would actually keep me at the clinic. Flash forward to the appointment, where the string of excruciating tests began. My OBGYN was concerned and I had every test done the gynecology floor could offer. A culture, STD panel, and various swabs. Unfortunately, all results were negative. Little did I know, that these gut wrenching symptoms were from a complication from my c-section in 2019. My doctor recommended an abdominal ultrasound. It felt like a special kind of hell as the technician kneaded into my belly for a good look at each organ. To this day, I’ve had seven ultrasounds and each time, I wish I swished four ibuprofen beforehand. The ultrasound showed no abnormalities. At this point, my OBGYN was convinced I had Endometriosis. My scans were clean, what else would it be? The only way to diagnose Endometriosis is to surgically check for lesions with a laparoscopy. My doctor mentioned most surgeons do not want to schedule a surgery until it is certain the pain won’t resolve on its own. She referred me to pelvic floor therapy for eight weeks. If therapy didn't help, we'd schedule the surgery. In total, I went through five weeks of physical therapy. I was told for Endometriosis patients, these exercises would alleviate the pain. At week three, my pain was at an all time high. I wouldn’t dare miss a window to take ibuprofen and the guilt of becoming less active with my toddler strongly set in. My body constantly ached and months of tight, gnawing back pain made its first appearance after a couple of PT sessions. I voiced my concerns to my physical therapist. I was then told… “Pain is normal for this therapy and it will get worse before it gets better.” “Could your skin be hurting because your bath water is too hot?” “I believe these are muscle spasms in your pelvis, not Endometriosis.” “This will not be a six week recovery. It will take months.” This is how I ended up at the ER. I had my first period since therapy started and combined with my existing symptoms, nothing would numb the sharp cramps surging through my body. I was admitted, given pain meds, and rolled in for an abdominal CT (x-ray). Next, I spent three hours waiting to get another abdominal ultrasound. They wanted to try a pelvic ultrasound, but I was reluctant. The pain meds were barely covering my symptoms, I couldn’t imagine something prodding around internally. I made the right choice too because the ultrasound felt like nails being dragged across my belly button. Back in my room, a doctor came in to let me know both the x-ray and ultrasound were clean. “The pain may be caused by your cycle and you should follow up with your OBGYN in case it is Endometriosis.” I couldn’t believe we sat in the ER for six hours, with toddler in tow, just to hear I should follow up with my doctor. What will happen when the pain medication wears off, I thought. The ER doctor recommended I take Ibuprofen with Tylenol. I sunk down in the chair and realized it was going to be a fight for anyone to believe me. However, this was just the event I needed to convince my OBGYN to schedule the laparoscopy to look for Endometriosis. My surgery was scheduled for April 4th. My dad came down to Tennessee to help with Trax and our hospital bags were packed. I prayed and prayed for them to find something. Anything. It didn’t need to be Endometriosis. I just needed to know what was causing this pain. I arrived at the hospital, they put me under, and did the diagnostic laparoscopy. Immediately, when I woke up I asked what they had found. A nurse replied, “They didn’t find anything, no.” Still out of it from the anesthesia, hot tears flooded my face and I threw a hysterical fit. What do you mean you cut me open and saw NOTHING? I remember them wheeling me out to the car where Trey was. I tried to fake some composure. I’m not sure how much of the crying rage he witnessed in the hospital room, but I didn't feel like embarrassing him more. For the rest of the evening, I sat in bed drifting in and out on painkillers wondering if I made the whole thing up. Am I the girl on tv who believed so badly she was in pain that her body mimicked her thoughts? Will I live this way well into my 30’s? The following morning, I rose and organized every cluttered corner of my room. I then landed deep in a sea of Endometriosis research and special treatment centers. “If a doctor isn’t very familiar with Endometriosis, it is possible for them to miss common signs like discoloration and lesions deeper than performed during a normal laparoscopy." That could be it. I frantically began to put together a case file for an Endometriosis specialist in Atlanta. A few days had passed and the incision pain had subsided. Although, my normal pelvic pain symptoms resurfaced. They fiercely settled back into my body. When my first period came back after surgery, it was then when the pain was no longer manageable with ibuprofen. It was like bulky river stones were stacked at the bottom of my spine. Cramps yanked hard at my pelvic muscles. We loaded up the car and headed for another ER. This time, we drove to a nearby town hoping for a better doctor. The nurses there were very kind. They ran similar scans to my previous visits and I finally allowed a vaginal ultrasound. If the surgeon didn't see something during the laparoscopy, maybe they will see it with this. The ultrasound was nauseating, but I held onto the fact it may uncover something new. Trey, Trax, and I waited in a hospital bed to hear the results. A women OBGYN entered the room and by the look on her face, you could tell she didn't have any answers. She referred me to a Gastroenterologist and mentioned the source of pain could be due to constipation from surgery or a digestive issue. I was livid. Then I thought to myself, "I made this whole thing up." We returned home and I struggled to get out of bed the next couple days because the pain continued. My mother-in-law had graciously come down to Tennessee to help with Trax after my dad headed home. She suggested we drive to Nebraska and find a new doctor. A couple days later, we made the 13 hour drive and I scheduled an appointment with a doctor in Lincoln. Thanks for coming by guys. It has been a tough 2022. My hope in writing this is to reach other mamas who have had c-sections and are struggling with extreme pelvic pain. My symptoms showed up slowly. My first symptom appeared a year post c-section. Please pay attention to your bodies, mamas.
On January 1st, I'll be posting Part Two. The last year has been a bitter ride of learning about c-sections and the impact they have on your body. Please read along if you or someone you know is experiencing similar symptoms and are looking for answers!
0 Comments
Your comment will be posted after it is approved.
Leave a Reply. |
Archives
April 2024
Travel bucket list:Countries visited: 5states left: 11Up next: |




 RSS Feed
RSS Feed
